Artemisinin and the Carbapenems: A Tale of Two Resistances
What's Hot in Medicine 2011
by David W. Sharp
A quick backward look at columns written over the past 20 years shows a dominance of epidemiological studies, clinical trials of both long-established drugs and new ones emerging from basic genetic research and reports of emerging new infectious diseases (often respiratory). For this latest column, I have picked a previously neglected area.
"Superbug" may not be a word much liked by the learned journals but it does at least recognize that bugs of all sorts have remarkable powers, not least the ability to acquire resistance to the synthetic agents that physicians throw at them. For example, MRSA has become a household word; it indicates methicillin resistance in Staphylococcus aureus, a Gram-positive micro-organism. A more recent concern is the emergence of resistance to antibiotics known as carbapenems among Gram-negative Enterobacteriaceae (which include Escherichia coli).
At #11 in the citation rankings this time is a worrying paper on a novel carbapenem resistance pattern associated with New Delhi metallo-ß-lactamase 1 or NDM-1 (K.K. Kumarasamy, et al., Lancet Infect. Dis.,10[9]: 597-602, 2010; total cites 148, latest count 40). The bacterial genes responsible for resistance are mobile in two senses: they jump from their natural hosts, and air travel ensures that the affected bacteria, carried by people who may not themselves be ill, spread worldwide.
This paper (#11) is a collaboration between workers in India, who report that in 2009 a significant proportion of instances of carbapenem resistance was associated with NDM-1, and the U.K. reference laboratory, where more than half the cases had a history of recent travel to India or Pakistan. Tested against 14 agents, these strains retained susceptibility to colistin and, to some extent, tigecycline, and that was all.
"...MRSA has become a household word; it indicates methicillin resistance in Staphylococcus aureus, a Gram-positive micro-organism. A more recent concern is the emergence of resistance to antibiotics known as carbapenems among Gram-negative Enterobacteriaceae (which include Escherichia coli)."
These findings, as the authors note, "potentially herald the end of treatment with ß-lactams, fluoroquinolones, and aminoglycosides," and the roster of new drugs in development is not densely populated.
The paper at #20 (A.M. Dondorp, et al., New Engl. J. Med., 361[5]: 455-67, 2009 ; total cites 219, latest count 34) sounds another alarm bell. For several years an artemisinin has been central to the management of malaria, the recommended strategy being to give the drug as combination therapy (ACT).
Artemisinin itself and four related compounds belong to the sesquiterpene lactone class of antimalarial drugs. Resistance to them would be a tragedy for global malaria control. From about 10 years ago hints of just such a problem have been emerging, and the findings in #20, from the Thai-Cambodia border where chloroquine resistance began over 50 years ago and then spread rapidly westwards, are worrying confirmation that all is indeed not well.
Dondorp et al. record delayed parasitological clearance for patients seen in Pailin, which is in western Cambodia. A letter in the same issue of the New England Journal of Medicine (H. Noedl, et al., 361[5]: 540-41, 2009) presents data supporting these findings. The World Health Organization has already set up a program to try and contain the spread of this artemisinin resistance. Failure would be a disaster because the new-drug pipeline for antimalarials is not exactly overflowing.
Last year WHO produced an excellent review ("Global Report on Antimalarial Drug Efficacy and Drug Resistance: 2000-2010") summarizing findings from older studies and ones set up specifically to look at resistance. It urges us not to talk of "ACT resistance" yet because clinicians and patients need not be anxious about the artemisinin part if the other arm(s) of the combined regimen remain active.
Containment of this problem must take account of several factors, including
counterfeit drugs, persistence of monotherapy with an artemisinin, and
non-compliance. A recent study from Kenya revealed that of almost 1,000
patients on ACT (here artemether-lumefantrine) only 64% were "probably
adherent" to the prescribed regimen (H. Lawford, et al.,
Malaria J.,10[1]: 281, 2011). Back in the laboratory, the hunt is
on for genetic markers of resistance (e.g., M.I. Veiga, et al.,
PLoS ONE,6[5]: e20212, 2011) and, again at the cellular and
molecular level, for resistance mechanisms.![]()
Mr. David W. Sharp, M.A. (Cambridge), formerly deputy editor of The Lancet, is a freelance writer in Minchinhampton, U.K.
| What's Hot in Medicine | |||
|---|---|---|---|
| Rank | Paper |
Cites This Period May-Jun 11 |
Rank Last Period Mar-Apr 11 |
| 1 | K.M. Flegal, et al., "Prevalence and trends in obesity among US adults,1999-2008," JAMA, 303(3): 235-41, 20 January 2010. [Ctrs. Disease Control & Prevent., Hyattsville, MD] *544VM | 119 | 2 |
| 2 | D.L. Ge, et al., "Genetic variation in IL28B predicts hepatitis C treatment-induced viral clearance," Nature, 461(7262): 399-401, 17 September 2009. [Duke U., Durham, NC; Schering-Plough Res. Inst., Kenilworth, NJ; Johns Hopkins U., Baltimore, MD] *494QB | 65 | 6 |
| 3 | T.S. Mok, et al., "Gefitinib or carboplatin-paclitaxel in pulmonary adenocarcinoma," New Engl. J. Med., 361(10): 947-57, 3 September 2009. [14 institutions worldwide] *490EI | 63 | 3 |
| 4 | S.J. Connolly, et al., "Dabigatran versus warfarin in patients with atrial fibrillation," New Engl. J. Med., 361(2): 1139-51, 17 September 2009. [12 institutions worldwide] *494QA | 53 | 7 |
| 5 | K.T. Flaherty, et al., "Inhibition of mutated, activated BRAF in metastatic melanoma," New Engl. J. Med., 363(9): 809-19, 26 August 2010. [9 U.S. and Australian institutions] *642HG | 51 | † |
| 6 | S. Jain, et al., "Hospitalized patients with 2009 H1N1 influenza in the United States, April-June 2009," New Engl. J. Med., 361(20): 1935-44, 12 November 2009. [Ctrs. for Disease Control & Prevent., Atlanta, GA] *518AI | 47 | 8 |
| 7 | P.C. Fong, et al., "Inhibition of poly(ADP-ribose) polymerase in tumors from BRCA mutation carriers," New Engl. J. Med., 361(2): 123-34, 9 July 2009. [7 U.K.. and European institutions] *467OS | 43 | 9 |
| 8 | L. Wallentin, et al., "Ticagrelor versus clopidogrel in patients with acute coronary syndromes," New Engl. J. Med., 361(11): 1045-57, 10 September 2009. [11 institutions worldwide] *492LP | 43 | † |
| 9 | R.J. Garten, et al., "Antigenic and genetic characteristics of swine-origin 2009 A(H1N1) influenza viruses circulating in humans," Science, 325(5937): 197-201, 10 July 2009. [26 institutions worldwide] *468FK | 41 | 4 |
| 10 | D.L. Thomas, et al., "Genetic variation in IL28B and spontaneous clearance of hepatitis C virus," Nature, 461(7265): 798-801, 8 October 2009. [13 U.S. institutions] *503OR | 40 | † |
| SOURCE: Thomson Reuters Hot Papers Database. Read the Legend. | |||
What's Hot In...
More Analyses
Featured Image
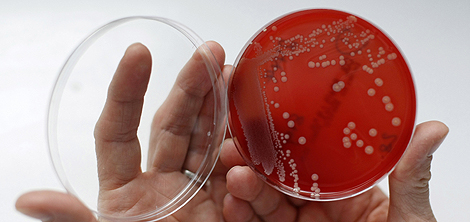
An employee displays MRSA (Methicillin-resistant Staphylococcus aureus)
bacteria strain inside a petri dish containing agar jelly for bacterial
culture in a microbiological laboratory. MRSA is a drug-resistant
"superbug", which can cause deadly infections.
REUTERS/Fabrizio Bensch.
